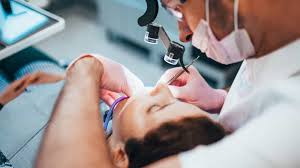
Choosing the right dentist is a fundamental part of maintaining long-term oral health and receiving quality care. A provider’s education, experience, and range of services can influence the patient experience and the effectiveness of treatment. Here’s more information on the qualifications to look for in a dentist:
Verify Education and Licensure
A practicing dentist holds specific degrees from accredited educational institutions. State boards issue active licenses, and they require strict adherence to local medical regulations. While general degrees provide basic knowledge, specific certifications demonstrate advanced training and indicate a higher skill level.
These official documents act as fundamental elements of professional practice. Licensure boards demand regular updates from active providers. Although a doctor passes initial exams, they must also complete ongoing education classes. The medical field advances quickly, and new clinical techniques require continuous learning.
Evaluate Experience and Focus
Clinical experience builds a dentist’s practical skill set; if you need a specific procedure, you seek a professional with a background in that exact area. General practitioners handle routine cleanings, but dental specialists perform targeted medical treatments. When you require specialized surgery, look for a seasoned professional and examine their past success rates. Some specialists focus on young children, and others handle adult surgical needs. A helpful provider explains their background clearly, and they share details about their daily work.
Assess Communication and Care
Clear communication stands as a key component of effective clinical practice. Since treatments involve specific medical terminology, the dentist should explain procedures clearly to patients. Here’s what you can expect as part of good communication and patient care:
- Clear explanations of medical terms.
- Written breakdowns of proposed procedures.
- Direct answers to clinical questions.
- Transparent protocols and processes.
These standard protocols make sure patients understand their care options. Good communication prevents clinical misunderstandings, and it establishes trust between parties.
Weigh Practice Quality
The physical facility reflects the overall quality of care; during your initial consultation, observe the facility’s sterilization methods and technology. A modern dental clinic uses current equipment, and the staff maintains a clean environment. You should also inspect the waiting room and observe the cleanliness of the clinical areas.
Evaluate the location’s operating hours and physical proximity; if the office is far away, you may miss routine appointments. Patients should also evaluate emergency medical protocols and ask about after-hours availability. If a distant clinic offers great care, long drives can create barriers and delay necessary appointments.
A reliable clinic maintains highly organized medical records. Modern medicine relies on digital tracking; the facility should store your files securely. The receptionist should manage schedules efficiently, and the clinical nurses should follow strict hygiene rules. Privacy laws protect your data; the dentist’s office should use secure software, and the staff should handle your information carefully.
Visit a Qualified Dentist Today
The process of selecting a provider involves methodical steps; you should thoroughly review education, experience, and communication standards. You should evaluate the facility and make sure the practice aligns with your needs. When you verify these specific details, you establish a strong foundation for your care and protect your oral health. Contact a qualified dentist near you to schedule your appointment today.