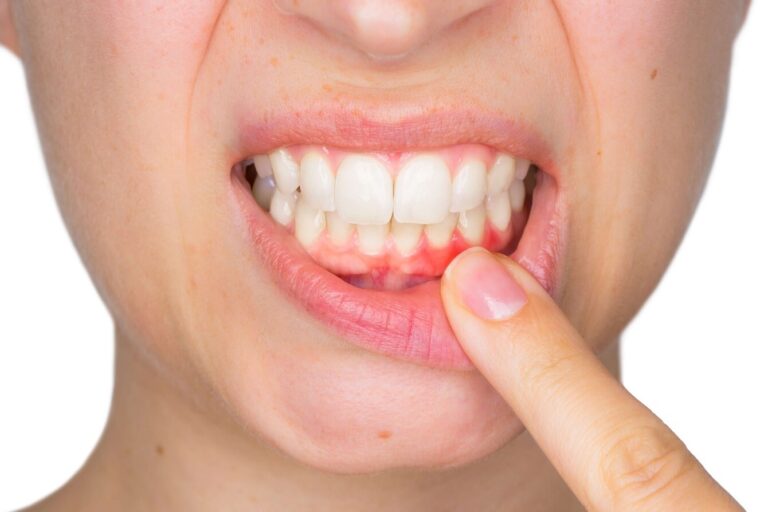
Gum recession separates the protective tissue from the teeth. This process exposes the roots underneath, and it leaves the teeth vulnerable to cavities. Because the roots lack a protective enamel layer, patients often experience pain, and they notice heightened sensitivity to hot or cold foods. About 88% of people over 65 have gum recession on at least one tooth, so practitioners frequently address this widespread condition. If the condition progresses, individuals risk bone loss, and their teeth might become mobile. Routine cleanings can become uncomfortable, and daily brushing may cause irritation. Early detection allows dentists to monitor changes, and they use periodontal probes to assess pocket depths. This can lead to gum treatments.
Identifying Gum Conditions
Several distinct factors cause gum tissue loss. Patients sometimes brush their teeth aggressively, or they develop thick dental plaque over time. While poor oral hygiene plays a role, many people have a genetic predisposition to thin gum tissue, and this trait makes them susceptible to recession. Tobacco use accelerates tissue damage, and abnormal tooth positioning can create stress on the gums. When periodontal disease develops, harmful bacteria infect areas below the gum line, and these organisms destroy the supporting structures. Certain dental appliances create friction, and they rub against the soft tissues continuously. Different gum treatments exist to help counteract this issue.
Exploring Gum Treatments
Dentists utilize multiple nonsurgical methods to manage early gum recession. Providers apply fluoride varnish to the teeth, or they recommend desensitizing toothpaste for home use. These products help reduce sensitivity, and patients often experience less discomfort over time. Scaling and root planing effectively clean deep beneath the irritated gums. Hygienists perform this deep cleaning under local anesthesia, and they place topical antibiotics directly into the periodontal pockets. Dental bonding offers another solution. The dentist camouflages the area with tooth-colored composite resin, and this material covers the exposed tooth root effectively.
Examining Surgical Procedures
Advanced gum recession often requires surgical intervention. Periodontists specialize in these procedures, and they routinely perform gum graft surgeries. During this operation, the surgeon takes tissue from the roof of the mouth or a donor source, and they stitch it over the exposed roots so that the teeth regain their protective covering. Guided tissue regeneration can repair severe damage, and osseous surgery reshapes the bone around the affected teeth when necessary. Minimally invasive techniques are available today, and patients usually recover in about two weeks while following detailed postoperative instructions for proper healing. Dentists monitor healing carefully, and follow-up visits ensure that the graft integrates successfully. Surgical management aims to protect the tooth root, reduce sensitivity, and restore gum health over time.
Find a Dental Office
Gum recession remains a permanent condition. Receding gums cannot grow back naturally, but appropriate therapies stop the progression of the disease. Although genetics influences oral health, individuals can reduce their risk by brushing twice daily and using antimicrobial mouthwash to control bacterial growth. Regular professional cleanings remove hardened tartar. Dentists monitor pocket depths carefully, and they use a periodontal probe to track changes over time. When individuals notice increased tooth visibility, they schedule prompt dental evaluations, and these visits allow practitioners to determine treatment options. Patients use soft-bristled toothbrushes daily to protect delicate tissues. Find a dental office in your area to maintain oral health.