An ankle wound is a physical injury to the lower extremity, and it requires careful monitoring to prevent worsening. Skin integrity is compromised during injury, allowing bacteria to enter the body more easily. Patients benefit from monitoring their healing process closely to avoid infections over time. Here is more information on these wounds and how to prevent complications:
What Is an Ankle Wound?
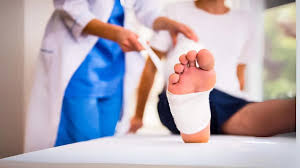
An ankle wound refers to any disruption of the skin or underlying tissues around the ankle joint. These injuries range from superficial abrasions to deep tissue ulcers, and they can affect mobility if left untreated. The anatomical location makes healing challenging, as the ankle constantly bears body weight. Skin in this area is relatively thin with minimal subcutaneous fat to protect the underlying bone.
Chronic conditions slow the body’s natural healing capabilities, and a minor scratch can evolve into a non-healing ulcer. The lack of blood flow to the lower extremities delays cellular repair, making the ankle particularly vulnerable to prolonged recovery. Skin repair requires a steady supply of nutrients, and poor vascular health disrupts this delivery system. A non-healing wound requires continuous clinical observation.
What Causes It?
Direct physical trauma is a primary cause of ankle injuries, and incidents like falls can damage the skin. Friction from poorly fitting footwear causes blisters, which can eventually rupture into open sores. Sports injuries often result in cuts or sprains. Structural deformities in the foot also alter walking patterns, placing abnormal stress on the ankle joint.
Medical conditions contribute to the development of chronic ankle sores. Poor circulation deprives the tissues of necessary oxygen, and diabetes often impairs nerve function in the lower extremities. Venous insufficiency causes fluid to pool in the legs, which breaks down the surrounding skin. Patients with underlying health issues face higher risks.
What Are the Symptoms?
A recognizable symptom is a visible break in the skin, and this may be accompanied by localized bleeding. Patients may experience persistent pain at the injury site. Swelling commonly occurs around the joint, making standard footwear difficult to wear. Clear fluid may drain from the wound bed, indicating active inflammation.
How Can You Prevent Complications?
Proper hygiene helps prevent infection, and patients should clean the area daily with mild soap. Applying a sterile dressing protects the exposed tissue, and changing this bandage regularly maintains a clean healing environment. Moisture management prevents skin breakdown. Patients should avoid applying direct pressure to the injury to prevent disruption of the healing process.
Monitoring the injury allows for early detection of potential problems. Patients benefit from inspecting the site during every dressing change. Wearing appropriate footwear reduces friction on the healing tissue, with specialized offloading shoes being beneficial for severe cases. Controlling blood sugar levels accelerates tissue repair in diabetic patients, and eating a balanced diet provides the necessary nutrients for recovery.
How Is Professional Care Beneficial?
Healthcare providers possess specialized training in tissue management, and they can accurately assess the severity of an injury. Clinicians use advanced diagnostic tools to identify underlying circulatory issues, and they prescribe targeted treatments for specific bacterial infections. Clinical debridement removes dead tissue from the wound bed, stimulating the growth of healthy new cells. Professional monitoring tracks healing progress over time.
Seek Professional Wound Care Today
Ankle wounds require continuous observation. Understanding the causes helps individuals minimize their physical risks, while recognizing symptoms may lead to faster clinical intervention. Basic preventive measures protect the skin from further damage, and professional treatment helps shorten the overall healing timeline. Schedule an evaluation to receive a personalized care plan today.