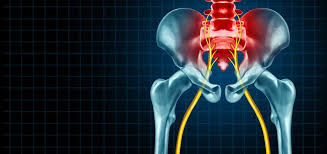
Chronic hip pain is persistent discomfort in or around the hip joint that lasts for three to six months or more. The discomfort may manifest in the groin, outer thigh, or buttocks, depending on the underlying issue. It typically develops from gradual wear and tear, repetitive stress, or structural changes within the joint itself. Living with this ongoing discomfort affects multiple aspects of daily life, extending beyond the localized physical symptoms. Chronic hip pain is a persistent condition that limits mobility, and it can significantly alter your daily routine. Understanding the underlying factors and recognizing the physical impact can help you effectively navigate the available professional management strategies.
Chronic Hip Pain Causes
Identifying the root of hip pain is a step in building an effective management plan. The hip is a complex ball-and-socket joint, and it is designed to withstand repeated motion and support the weight of the body. Over time, various factors may disrupt its function and create ongoing stiffness. Several common conditions frequently contribute to persistent hip discomfort:
- Osteoarthritis: This condition involves the gradual breakdown of articular cartilage, which typically provides a smooth, frictionless surface for joint movement.
- Bursitis: The bursae are small fluid-filled sacs that cushion the bones, muscles, and tendons. Inflammation of these sacs often causes noticeable friction during movement.
- Repetitive Strain Injuries: Repetitive motion and overuse can irritate the thick bands of tissue connecting muscles to bones around the hip.
- Previous Injuries: Old fractures, dislocations, or labral tears can alter joint mechanics over time, leading to prolonged issues.
- Referred Discomfort: Sometimes, issues originating in the lower back, such as a pinched nerve, radiate into the hip area.
Physical and Functional Effects
Ongoing hip discomfort creates concrete physical limitations that affect overall independence. Individuals frequently experience a reduced range of motion, and this alters their natural gait and balance. This mechanical shift places excess strain on the lower back and knees as the body unconsciously attempts to compensate for the compromised hip.
The condition limits your overall flexibility, so simple tasks like tying your shoes often become difficult. Activities that require prolonged sitting, standing, or walking up stairs can trigger sudden stiffness and radiating discomfort. This physical tension frequently disrupts normal sleep patterns. Finding a comfortable resting position becomes challenging, leading to sleep deprivation and fatigue that, in turn, further affect daytime function. The combination of restricted movement and persistent fatigue directly impacts the ability to work, participate in hobbies, and manage routine household responsibilities.
Professional Management and Treatment Options
Addressing ongoing hip discomfort requires a structured, multi-disciplinary approach. Pain management and orthopedic specialists are physicians with additional training in treating and managing complex pain or orthopedic conditions. These specialists provide a comprehensive framework to support your mobility and daily function; following a thorough evaluation, which may include physical exams and imaging tests, they are able to recommend specific interventions.
Standard professional management strategies include:
- Walking Aids: Using devices such as canes or walkers can provide additional support, improve stability, and help maintain mobility.
- Medication Management: Specialists may suggest specific non-steroidal anti-inflammatory drugs or targeted joint injections to address localized inflammation.
- Lifestyle Modifications: Adjusting daily routines and maintaining an optimal weight can drastically reduce mechanical stress on the joint.
- Activity Modification: Transitioning to low-impact exercises, like swimming or stationary cycling, helps maintain cardiovascular health without overloading the hip.
Ask your doctor any questions about your condition or the recommended treatment.
Talk to a Specialist Today
Addressing persistent joint discomfort promptly can help preserve your mobility and improve your daily function. A dedicated specialist can evaluate your specific symptoms and review your medical history, and they are able to design a targeted plan for your unique physical needs. Contact a qualified healthcare professional today to discuss your options and regain control over your physical well-being.