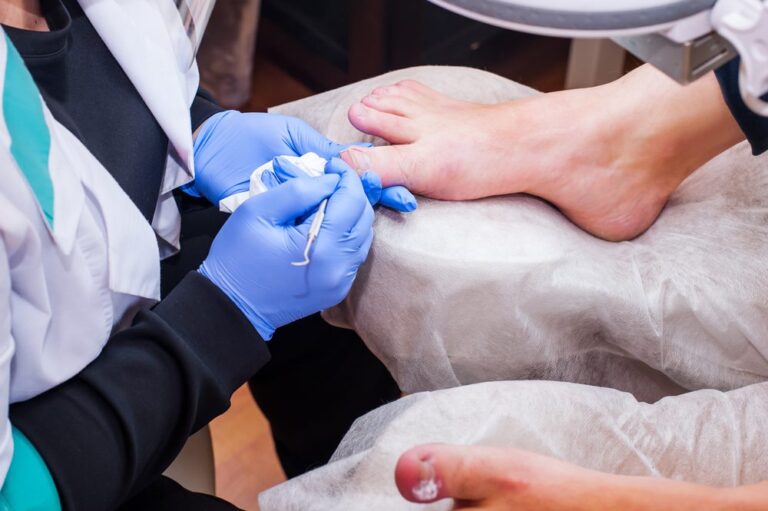
Recurring ingrown toenails can disrupt normal daily activities. Swelling may occur, and toe pain limits movement. If pus oozes, you must seek care. Because complications may arise quickly, prevention matters.
Symptoms of the Condition
Red or darkened skin signals a problem, and this change develops gradually or suddenly. Your toe feels warm, and pain develops quickly. As swelling worsens, blood or clear fluid can ooze around the nail. Pus may appear white, yellow, or bloody; these signs need prompt care. If you ignore symptoms, you may have recurring ingrown toenails. Tenderness around the nail border is common. You might also see inflammation and tight, stretched skin, which makes it painful to wear some shoes.
When redness spreads or tissue feels hot, medical advice is needed quickly. Constant toe pain can limit walking or daily activities. Even a lightweight blanket or bedsheet pressing on the area may create discomfort at night, so keep pressure off the toe. Pressure may cause sharp pain, so wear sandals or open shoes. Because untreated symptoms can escalate, early detection matters. Notice these signs quickly, and manage the condition.
Causes Behind the Problem
Incorrectly cut toenails lead to various problems. If you trim your toenails too short or round off the corners, nails grow unevenly and press into the skin, raising the risk of ingrown toenails. People might wear improper shoes, and tight footwear creates pressure. Pressure can happen while running or walking long distances. Narrow or pointed shoes squeeze the toes together, forcing the nail edges down and causing irritation. Trauma, like stubbing your toe, can change nail growth direction and raise the risk of ingrown nails. Your natural toe shape matters; some people nail shapes increase the risk. Tissue grows around nails, or nails grow too large for the toe. Nerve damage can stop you from sensing symptoms right away.
Treatments for the Toe
Warm water soaks work well, and they are an option for relief. Treatment steps include:
- Soak the affected toe in warm water with Epsom salt twice daily.
- Keep the toe dry at all other times to prevent excess moisture.
- Apply an antibiotic cream and cover the toe with a bandage.
- Gently lift the nail edge and place clean cotton or dental floss under it.
- Change the cotton or floss daily to maintain cleanliness.
- Choose roomy, comfortable footwear.
Epsom salt can soften the nail and skin. After soaking your foot, keep it dry and wear roomy shoes to limit pressure on the area. Your provider may gently place cotton or dental floss underneath to guide the nail’s growth away from the skin. Change the cotton or floss each day, even if your toe feels better. Pain relievers ease discomfort, and over-the-counter medications like ibuprofen or acetaminophen can be used. If pain persists or the infection is severe, a nurse or doctor will partially remove the nail for quick relief. Never try to remove the nail yourself. Wearing sandals or open shoes lowers pressure, and they allow the skin to heal without irritation.
Prevent Recurring Ingrown Toenails
Prevention requires correct nail trimming. Cut nails straight across, and never round the corners. Before you cut nails, always use clean trimmers. Avoid repetitive toe trauma entirely. Wear properly fitting shoes, and protect your feet daily. Proper footwear prevents excess pressure. You should avoid tight shoes, and loose shoes offer little support. While you heal the toe, caution matters, and consistent care prevents recurrence.