What To Expect During a Root Canal Procedure
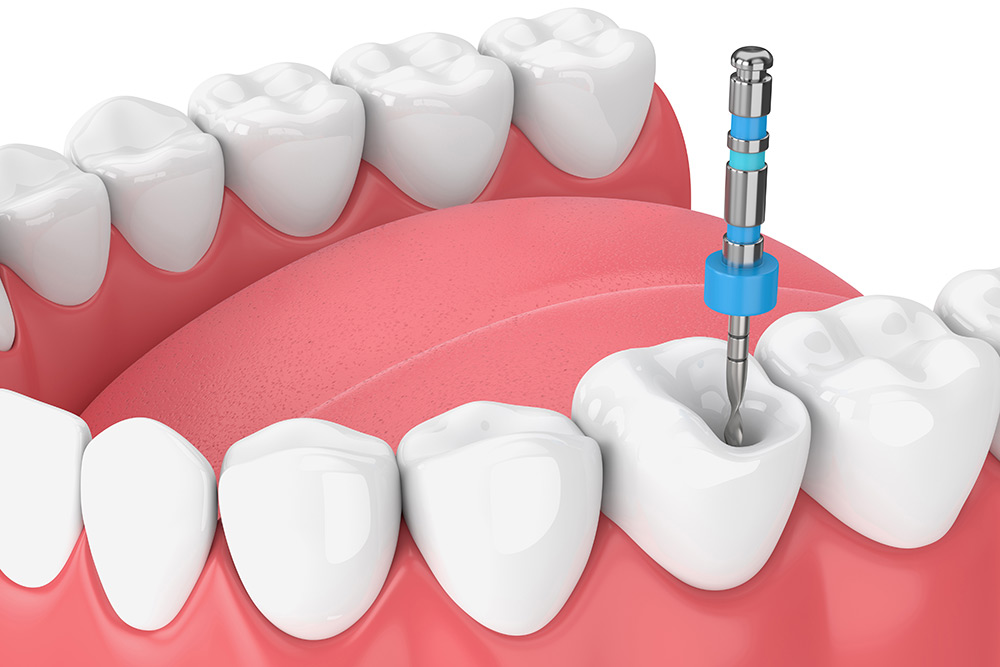
Root canal therapy treats a severely damaged or infected tooth. The procedure removes infected tissue, and it preserves the natural tooth structure. When patients experience severe decay, providers evaluate the area, and they recommend treatments to stop the infection. The treatment helps patients avoid tooth extraction, and it maintains oral health. Providers clean the inside of the tooth, and this step prevents bacteria from spreading. Because untreated decay causes pain, intervention relieves discomfort, and patients retain their teeth.
Procedure Overview
Root canal therapy targets severe decay or infection inside the tooth. Providers remove the inflamed pulp, and they disinfect the internal chamber. Since the pulp contains nerves and blood vessels, extracting it stops pain, and the empty space is thoroughly cleaned. The provider shapes the canals, and a rubber-like material called gutta-percha fills the space. This biocompatible material seals the tooth completely, and it prevents future infection. After the canals are filled, the provider places a final restoration, and the tooth regains its normal function and appearance.
Symptoms Indicating Treatment
Several signs suggest a tooth may require root canal therapy. Severe tooth pain occurs during chewing, or it appears when patients apply pressure to the area. If hot or cold temperatures cause lingering sensitivity after prior dental work, the pulp may be damaged, and providers evaluate the tooth promptly. Swollen or tender gums near the affected tooth indicate infection. A recurring pimple-like bump might appear on the gums, and this symptom signals persistent bacterial growth. Because nerve damage can darken a tooth, unexpected discoloration warrants professional examination, and providers determine whether treatment is necessary. Cracks or chips in a tooth expose the pulp, which increases infection risk, and early recognition allows timely intervention.
Treatment Steps
Root canal therapy follows several carefully structured steps to restore the tooth. Providers first administer local anesthesia, and this numbs the surrounding area for comfort. Once the tooth is numb, the provider creates a small opening to access the pulp chamber, and specialized instruments remove the infected tissue. The canals are then cleaned thoroughly, and all bacteria and debris are eliminated. Because the procedure targets the source of infection directly, the tooth structure is preserved, and normal function is maintained after restoration.
Next, the canals are filled with gutta-percha, which seals the space and prevents reinfection. The provider then restores the tooth with a filling or crown, and the restoration restores chewing ability and appearance. Although a standard filling works in some cases, many teeth require a full crown, which strengthens the structure beneath it. Patients leave the office with a sealed tooth, and normal function is restored. When complete, the restored tooth looks natural, and it performs like surrounding teeth.
Get a Root Canal
Root canal therapy effectively saves severely decayed or infected teeth. The procedure removes infected pulp, and the final restoration restores normal chewing function safely. Recognizing symptoms such as prolonged sensitivity, gum swelling, or discoloration allows patients to seek prompt care; treatment stops the infection from spreading. By sealing the tooth and restoring its structure, providers prevent further complications, and patients avoid extraction. Timely intervention eliminates pain, preserves the natural tooth, and maintains oral health for years.
- How to Start Practicing Tai Chi at Home: A Complete Beginner’s Guide
- The Benefits of Laminate Flooring: Durability, Cost, and More
- The Top 5 Commercial Painting Companies in Southern California
- Best Practices for Designing Intuitive Mobile Radio Buttons
- Don’t Wait for a Backup: The Benefits of Regular Drain Care