The Connection Between Arthritis and Joint Mobility
Arthritis can directly affect joint mobility by causing pain, stiffness, swelling, and a reduced range of motion over time. As the condition progresses, simple movements may become more difficult, affecting daily comfort and physical function. Here is a closer look at the connection between arthritis and joint mobility:
Changing Joint Movement
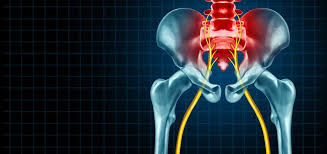
Arthritis changes the physical structure of the affected joints in several ways. While healthy joints rely on intact cartilage for painless movement, arthritic joints suffer from ongoing tissue damage. The protective cartilage eventually wears away completely, and the underlying bones begin to rub directly against one another. When the human body detects this internal mechanical friction, it automatically triggers a biological immune response. The resulting swelling expands the surrounding soft tissue, and the entire joint capsule tightens significantly as a direct result.
Limiting Daily Mobility
Limited joint mobility can significantly disrupt routine activities and hinder an individual’s overall well-being. Here are some of the key ways in which restricted movement impacts daily functioning:
- Difficulty with Physical Tasks: Simple activities such as climbing stairs, walking, or lifting objects become increasingly challenging, leading to a more sedentary lifestyle.
- Impaired Work Performance: Jobs requiring physical exertion may become unmanageable, potentially reducing productivity or necessitating a change in occupation.
- Reduced Independence: Tasks that individuals once performed independently, such as dressing, cooking, or cleaning, may now require external assistance.
- Chronic Discomfort: Persistent pain associated with limited mobility can affect focus, mood, and overall well-being.
- Social Isolation: Restricted movement may prevent participation in social activities, contributing to feelings of loneliness or depression.
These limitations underscore the need to maintain joint health and seek timely interventions to preserve mobility and independence.
Identifying Common Types
Although doctors classify over 100 variations of the disease, osteoarthritis and rheumatoid arthritis are the most common in the general population. Osteoarthritis generally develops from natural mechanical wear, but rheumatoid arthritis primarily stems from an abnormal immune response. A patient may develop osteoarthritis after a severe sports injury, and the joint damage worsens if they do not seek medical care. These specific conditions cause severe joint inflammation. While osteoarthritis primarily affects large joints like the knees, rheumatoid arthritis generally affects the smaller joints in the hands.
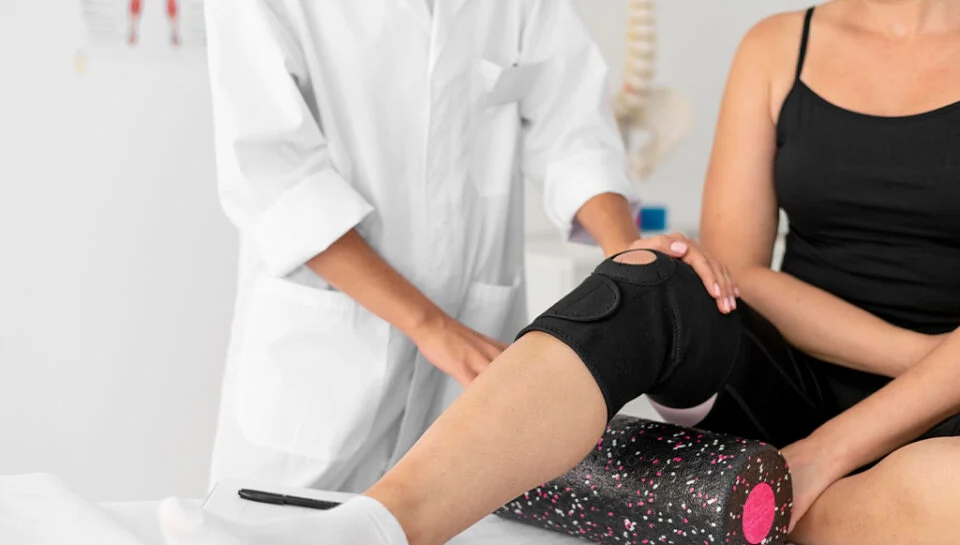
Supporting Better Mobility
Maintaining mobility with arthritis requires a combination of lifestyle adjustments, therapeutic interventions, and assistive strategies. Here are key methods to support joint function and reduce discomfort:
- Exercise Regularly: Low-impact activities such as swimming, walking, or yoga can strengthen muscles around joints and improve flexibility.
- Maintain a Healthy Weight: Reducing excess weight helps alleviate pressure on weight-bearing joints.
- Use Assistive Devices: Canes, braces, or shoe inserts offer more joint support and improve stability during movement.
- Engage in Physical Therapy: A physical therapist can provide individualized exercises and techniques to enhance the range of motion and functionality.
- Apply Heat or Cold Therapy: Heat soothes stiff joints, while cold reduces swelling and inflammation.
Incorporating these strategies can help individuals with arthritis better manage their symptoms and maintain an active and independent lifestyle.
Get Help for Arthritis Today
Implementing practical strategies can help individuals with arthritis alleviate pain, improve joint functionality, and enhance their quality of life. Taking proactive steps toward symptom management helps individuals to maintain an active and independent lifestyle. Contact a qualified orthopedic specialist near you to schedule your arthritis appointment today.
- How to Start Practicing Tai Chi at Home: A Complete Beginner’s Guide
- The Benefits of Laminate Flooring: Durability, Cost, and More
- The Top 5 Commercial Painting Companies in Southern California
- Best Practices for Designing Intuitive Mobile Radio Buttons
- Don’t Wait for a Backup: The Benefits of Regular Drain Care